In Part 1 of our three-part series on falls prevention technology, we reviewed the role of technology in falls prevention and discussed how you can evaluate available technologies. Part 2 now focuses on how to integrate technology into a comprehensive fall prevention program. Part 3 will address how to optimize your use of technology.
Most of the information in this blog derives from a Posey® white paper1 written by Cynthia Saver and published by TIDI Products, LLC.
Integrating Falls Prevention Technology: Steps for Success
Once a hospital or long-term care facility evaluates and selects a specific falls prevention technology (refer to Part 1), the technology must be integrated within the organization’s overall fall prevention program. Below is a list of steps intended to help guide this process.
Integrating technology into a fall prevention program:
- Obtain buy-in
- Form a team
- Establish goals and a timeline
- Create a plan
- Provide education
- Monitor and follow up
Note that the evaluation of a technology and its subsequent integration into a comprehensive fall prevention program are complementary. Decision makers should therefore be mindful of the integration process when evaluating a technology for purchase.
Building Consensus and Strategizing
Step 1: Obtain buy-in. Before starting a fall prevention program that includes technology, gain buy-in from top leadership by presenting fall data for the organization, national data on the costs of falls, and how a prevention program can offset costs. For example, the Centers for Medicare & Medicaid Services does not reimburse for costs associated with falls that occur in hospitals. Involvement of top leadership facilitates buy-in at all levels, including unit leaders and staff.
Step 2: Form a team. Key members for a fall prevention team include nurse managers, staff nurses, advanced practice nurses (e.g., clinical nurse specialists, nurse practitioners), occupational and physical therapists, pharmacists, quality experts, and representatives from senior management.

Other potential members include an environmental services representative, a physician, and a bioengineer, who can address safety and ongoing maintenance of technology. The informatics department can help integrate documentation of fall prevention interventions, such as use of technology, into the electronic health record. Innovative organizations have also added former patients and family members to the team for their perspectives.
The team should understand the purpose of the program and promote just culture principles, such as not blaming others if a fall occurs. Most important, the team must have the authority to make decisions.
Step 3. Establish goals and a timeline. To establish goals, the team should perform a self-assessment by analyzing fall data and conducting a SWOT analysis, which looks at strengths, weaknesses, opportunities, and threats. Prior to purchase, the team should assess the value of technology and users should test the new product. Having a timeline will help keep the team focused.
Step 4. Create a plan. Many plans include bundles of interventions. Some of these interventions can be universal, meaning applicable to all patients, such as interventions addressing prevention of accidental falls related to environmental risks like poor lighting, cluttered rooms, and multiple cords (shown below, left). However, bundles must be adapted to accommodate patients’ individual needs.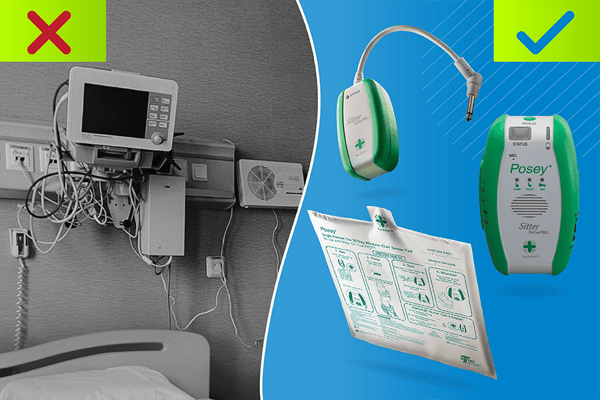
Bundles typically include several strategies that may be part of a larger plan. One organization, for instance, uses yellow fall bundle interventions (e.g., wristband, door magnet), family notification and involvement in care (if they are able), bed alarms and chair alarms application, and scheduled environmental checks that can activate physician notification.2
Shown above, right, the Posey Sitter On Cue PRO™ Platform from TIDI Products is a newly available, clutter-reducing technology that uses an alarm, a wireless chair sensor pad, and a wireless nurse call adapter. This innovative falls prevention technology solution features Tap-2-Pair™ technology, which establishes a wireless connection with a simple tap. Visual and audio indicators confirm device pairing.
Education and Monitoring
Professional development staff have multiple demands, such as staffing shortages, that make providing education challenging. Therefore, the level of educational support the manufacturer will supply is crucial. In addition to in-person instruction, it is helpful to ask about supplemental resources such as videos and webinars. Often these resources can be embedded into an organization’s existing education platform for ease of use.
Step 5: Provide Education. Education about a new technology is an ideal time to reinforce the overall fall prevention program. All staff who will be in contact with the technology, such as nurses, nursing assistants, therapists, and transport staff, need to be educated. So do non-direct care staff who will be in the patient’s room, such as dietary and environmental services, and staff who will be interacting with the patient, such as speech language pathologists. Failure to educate can lead to more false alarms, such as when a transporter moves the patient from the bed to the wheelchair.
Step 6: Monitor and follow up. Monitoring includes ongoing patient assessment and adjustments to the care plan as needed, as well as effectiveness of the technology and the overall fall prevention program, so that policies and protocols can be refined as needed. This monitoring can help reinforce desired behavior. Share fall data at least monthly and discuss areas for improvement. Encourage staff to share success stories related to how the technology prevented falls, as well as near misses that may provide valuable lessons.
For a more detailed discussion of each of the steps for integrating technology into a fall prevention program, you can download our white paper here.
We also invite you to learn more about our new Posey Sitter On Cue PRO wireless technology solution for falls prevention.
1 Saver, C. Role of Technology in Falls Prevention: A Patient-centered Approach [White Paper (2022), TIDI Products, LLC].
2 Opsahl AG, Ebright P, Cangany M, Lowder M, Scott D, Shaner T. Outcomes of adding patient and family engagement education to fall prevention bundled interventions. J Nurs Care Qual. 2017;32(3):252-258. doi:10.1097/NCQ.0000000000000232
